Covid19 brings chaos and horror to the Subcontinent
India thought it had escaped the worst. It was wrong.
By Vivek Y. Kelkar, Mumbai
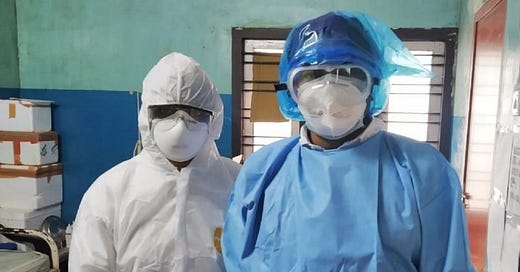
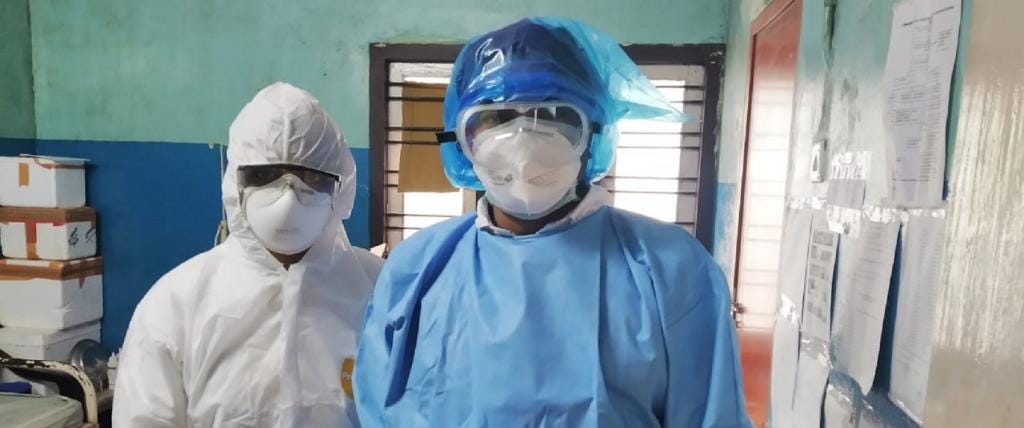
Last year, during the first wave, India seemed to be one of the world’s success stories. Now it is chaotic, terrified, and helpless. Cases are zooming up. Patients and families are turned away, sobbing, from hospitals that have no beds. On social media, the clamor for oxygen cylinders, ventilators, and antibiotics grows louder and more desperate. The government dithers over lockdowns. Political rivals point fingers. Television presenters scream of government incompetence. Vaccination centers run out of vaccines. Despair and death are ubiquitous.
India has a lot going for it, or so it seemed, until two months ago. We crowed that we had the world’s largest vaccine manufacturing capacity; ours is a large and well-developed pharmaceutical sector. Our doctors and hospitals, in the major cities at least, are truly world-class. We have 7,000 metric tons of medical oxygen manufacturing capacity. In the first few weeks of February, many a recipient praised our vaccination program; Staggering the doses seemed to work, even if some critics disputed its logic.1
But as the second wave of the virus hit, in early March, India’s capabilities were put to the test. Reality hit hard. Two days ago, India had 16.3 million confirmed cases, or so the government said, out of a global total of 144.7 million. But India had 332,921 new cases of Covid19 on that day alone—the highest single-day tally anywhere in the world since the pandemic began.
It’s the Modi government’s fault, scream baiters of the country’s prime minister—he dared hold elections and allowed religious gatherings during a pandemic!
Was the government napping? Did it lift restrictions too soon? Was the public too eager to conclude the pandemic was over and India had been spared? Did it abandon masks and social distancing prematurely?
Or did new strains of the virus appear and spread all over India, which was simply too chaotic and unprepared to cope with this virulent onslaught? Was Modi’s central government alone to blame, as many of its critics claimed, or did officials at both the central and local levels fail to plan?
All of the above!
Two days ago, according to government statistics, 13.2 million had recovered while some 187,000 had died. The government statistics are a lie, screamed many across social and other media. Far more had died—you could tell from the crowds at the cremation and burial grounds; they were vastly larger than that, they said. Neither the government figures nor this anecdotal evidence, splashed over social media, could be proven. Or disproven.
The government claimed 135 million people had received at least the first dose of the vaccine by April 22 (the global number was 937 million) and 20 million Indians had received both doses. But even in the major metropolises, such as Mumbai and Delhi, the vaccination centers were running out.
In cities like Mumbai, the local authorities have some kind of system in place. In the affluent Mumbai suburb of Versova, Ernest Pinto and his wife Charmaine, both in their sixties, quarantined at home during their illness. The local municipality called them every morning to ask about their symptoms and doctors spoke to them by video.
But the Pintos were lucky to live in Mumbai and to be only mildly ill. In other parts of the country, particularly in Uttar Pradesh, Karnataka, and Tamil Nadu, thousands of severely ill people have discovered there are no hospital beds and no oxygen. Ambulance services have been stretched to the breaking point. Patients arrive at hospitals in rickshaws, only to be turned away. On television and social media, we have been flooded with scenes of desperate families crying.
Why is a question with no easy answers.
The mutants
All viruses mutate. But SARS-CoV-2 seems to be spectacularly good at it. In early April, India’s health ministry announced it had detected 771 variants of the coronavirus in India. This includes the so-called double mutant, B1617, as well as strains previously discovered in the UK, Brazil, and South Africa. Some feared B1617 was more infectious and skillful at evading vaccines: Many who had been vaccinated, with both doses if needed, nonetheless reported symptoms. Among them was the former prime minister, 88-year-old Manmohan Singh. He was in stable condition as of Thursday. There has been no word about which strain infected him.
The health ministry warned that the B1617 mutant might spread more rapidly than other variants because one of its mutations, L452R, changes the part of the spike protein that interacts with ACE2 molecules on the surface of the cell. This is where the virus binds; the mutation may allow the virus to gain a more stable foothold.
Researchers worldwide are studying this mutation, among the many others that have surfaced. Worries B1617 might hamper vaccine efficacy are growing. Preliminary studies have suggested it may be able to evade much of the human immune system. What’s more, it is less susceptible to preexisting antibodies.
It is not yet certain that the vertiginous rise in cases in India is owed to new variants, but an Indian health ministry official told the Cosmopolitan Globalist that the ministry strongly suspects it is so.
The insoluble economic dilemma
Just over two weeks ago, Uddhav Thackeray, the chief minister of Maharashtra, one of the worst-affected states, went live on television and put the government’s dilemma baldly: “On the one hand, there is a public sentiment, but on the other hand, there is an outbreak of coronavirus, in which case if you want to win this battle, you have to go through some hardships.” He was referring to pleas from businesses to avoid a complete lockdown, and alluding to a social media contingent that insists lockdowns don’t work and only hurt the poor.
During the first wave, much of the media, domestic and global, criticized the Modi government’s decision to impose a lockdown on half a day’s notice. Then, as now, the government faced the problem of vulnerable migrant workers who in the event of a lockdown would be forced either to stay in the cities without income or return to their towns or villages in overcrowded transport, bringing the virus with them. Modi’s government, widely criticized for having declared a lockdown last year with disruptive speed, seemed unwilling to hurt the economy again, especially since it was had only just been showing signs of revival.
The plight of migrant workers from rural India, the largest part of the labor force in urban areas, was not the only matter on the government’s mind. Small- and medium-sized businesses form the backbone of India’s manufacturing and service sectors. They too had to shut shop last year, leading to severe unemployment and industrial shortages.
So the government dithered, at both the central and the local levels, avoiding lockdown until it was too late and the crisis had reached monumental proportions. Even then, some governments, such as those in the northern Indian state of Uttar Pradesh, refused to impose lockdowns, or even milder restrictions on people’s movements. As late as April 20, the state government declared it was “working with full commitment to control coronavirus infections.” It proclaimed it was developing a strategy for testing and tracing. It would also be tracking a “continuous supply of oxygen along with the availability of ICU beds for prevention of Covid19.” The government in Maharashtra called for a curfew in the evening and at night, but confronted ridicule on Twitter and an infuriated retail and small business sector.
Finally, yesterday, stringent lockdowns were imposed on most of India. The problem with the labor force remains, however; migrant workers are refusing to stay in the cities. They crowd railway stations as they try to return to their small towns and villages. This dilemma is insoluble.
Does India have the resources?
The question now is whether India, with more than 1.3 billion people, has the resources to cope with the greatest infectious disease crisis seen in a century. It should have been apparent from the outset (and indeed, many warned of it) that by virtue of population alone, the pandemic in India would be an unspeakable humanitarian disaster.
India’s governing elite has much to answer for. By mid-February, overcrowded railways and buses had resumed normal service. Markets, malls, cinemas, and restaurants were jam-packed. DJs were in demand at the nightclubs; party-goers danced the evenings away in merry abandon. Between March and mid-April, India held state-level elections, with mass rallies and occasional violence. Hindu religious festivals and gatherings proceeded uninterrupted, with hundreds of thousands pressing and shoving, cheek-by-jowl, to dip themselves in the holy rivers and wash away their sins.
A few weeks ago, the chief minister of Uttar Pradesh, Yogi Adityanath, claimed yoga and deep breathing would protect people from the virus (which he contracted last week). Uddhav Thackeray, the chief minister of Maharashtra, meanwhile blamed the people for their plight: They had refused to stay indoors and stubbornly worn their masks around their chin.
In truth, neither central nor state governments planned adequately for a second wave, even though the medical profession warned both it was inevitable. They failed to augment supply chains for oxygen cylinders, procure ventilators, or manufacture antibiotics. No one in government made plans for this at all.
Thackeray rightly argued that even if beds and quarantine facilities could be increased by requisitioning every private hospital and even hotels, the number of doctors and trained medical personnel would remain finite. But yesterday, the only images we saw in the news were those of helpless people racing around, desperate, trying to secure medical resources—and these were not available. No effort had been made to augment the country’s supply of medical oxygen. Nor had anyone created dedicated emergency supply chains; or at least, none were visible, and no regulator has made any claim to the contrary.
Only in the second week of April, when numbers began skyrocketing, did governments at both the central and state levels react. Last week, in Uttar Pradesh, the government announced it would set up three new oxygen plants within days. It did not answer the question, “Is that feasible?” On April 20, virus-stricken Yogi Adityanath announced the opening of a dedicated Covid hospital with a capacity of 225 beds and 700 more to come; a suite of private medical facilities would be impressed into service. Three days later, it is clear this will not be enough.
Thackeray declared private laboratories would add to the government’s testing capacity. He claimed 104 private laboratories and 125 public sector laboratories were being set up to conduct tests, but where their equipment would come from was unclear.
Everywhere, across the country, the situation was exactly the same.
Hospitals have gone to court against the government in Delhi, demanding it supply them with oxygen. Their patients are dying from shortages. The High Courts and Supreme Court have demanded the government build resources on a war footing, even as India’s agitating farmers continue to block the highways that provide access to the capital. The farmers aren’t deliberately blocking trucks carrying oxygen, but the trucks have been delayed at the city’s borders because sections of the highway are impassable, thanks to the farmers’ agitation. Police and regulatory bodies across the states that border Delhi don’t coordinate with each other or with their counterparts in the capital. Yesterday, Max Healthcare, which runs two hospitals in Delhi with some 700 patients, sent out an SOS tweet: It had been waiting seven hours for fresh oxygen supplies.
Meanwhile, the government declared a special green zone, a dedicated railway corridor for freight trains to supply oxygen across the country. It is in talks with India’s massive steel manufacturing and petrochemical sector to augment India’s medical oxygen capacity (for many of these industries, oxygen is an intermediary stage or a byproduct). The country’s largest petrochemical manufacturer, Reliance Industries, run by one of the world’s richest men, Mukesh Ambani, says that it is transforming its oxygen-generating process to produce medical grade oxygen. The country’s largest fertilizer manufacturer, IFFCO, has followed suit.
The health ministry had argued India was self-sufficient in oxygen. But it has discovered there is a big difference between theoretical self-sufficiency and being in possession of detailed, coherent plans to coordinate the supply of oxygen to thousands of hospitals spread across the India’s huge landmass, from the north to the south.
Six months ago, news stories called India the world’s vaccine manufacturing capital. Some said India supplied 60 percent of the world’s vaccines. But the data that has now emerged tells a different story.
It’s true that India has administered 135 million doses of vaccine to its population, lagging only the US, which has administered 213 million doses, and China, which has administered 195 million. Globally, 929 million doses have been administered. India contributed about 21 percent of these doses, although this figure includes the doses it has given to its own population. According to India’s external affairs ministry, India has exported 66 million doses to 94 countries, about 16 percent these gifts, the rest part of the Serum Institute of India’s contract with Covax.
But despite self-congratulation about the size of India’s vaccination sector and its exports, the numbers don’t add up to the numbers needed to fight the pandemic. India’s contribution to the world’s vaccine supply may be 60 percent, but its contribution to the supply of vaccines that prevent Covid19 is nowhere near that. The 60 percent figure includes India’s contributions to UNICEF’s childhood vaccination program: India supplies vaccines against polio, measles, and diphtheria—not vaccines against Covid19.
There is nothing to be ashamed of in producing vaccines that prevent polio. To the contrary. But it seemed to occur to no one that this capacity would not translate into the ability quickly to manufacture Covid19 vaccines. The techniques and the equipment are not the same. Only seasonal influenza vaccines are made in a sufficiently similar way that manufacturers can quickly repurpose their facilities to make Covid19 vaccines at scale. And unfortunately, India is not a giant in flu vaccine manufacturing. India makes few influenza vaccines because there is very little demand for it in India. Flu shots, typically, are marketed in developed countries.
Clearly, the Indian government miscalculated. A survey published by the WHO in January noted that manufacturers in developing countries—such as India—had augmented their flu vaccine capacity, but still produced only 17 percent of the world’s supply. The rest is made in developed countries. Only three Indian companies—CPL Biologicals Pvt. Ltd., the Serum Institute of India, and Zydus Cadila—are established influenza vaccine manufacturers. Contributions from new vaccine makers, like Bharat Biotech, raised the number a bit, but nowhere near enough to make the switch to Covid vaccines and fulfil India’s demand. If you add old and new capacity together, India could at best make 800 million doses a year. India’s population is 1.3 billion.
India needed an external supplier. But much like the EU, India’s health ministry fell prey to hubris and miscalculation. In November 2020, the health ministry announced that India might not need the Pfizer vaccine. It publicly doubted the multinational’s ability to manufacture in India. The government fixated on concerns about price and liability, even though neither were an insurmountable obstacle. Pfizer withdrew its application last January, just weeks after submitting it.
Throughout January and February, the Indian government failed to grasp reality. It browbeat both Bharat Biotech and the Serum Institute to lower the price per dose below the US$3 recommended by Covax. But it failed to make grants or funds available to manufacturers. And it failed to contract for the amount India needs.
It wasn’t until mid-March, when vaccine shortages became obvious, that the central government responded, first, by creating a six-member inter-ministerial panel to build more manufacturing capacity through a special clearance that allowed manufacturers to rush through requests to repurpose their facilities. But manufacturing still lagged demand.
The government then approved the Sputnik V. Russia entered agreements with six Indian pharma companies, including Dr. Reddy’s, one of India’s largest, to make 850 million doses of Sputnik V. But no one knows when, exactly, they will hit the market; the latest word is that they won’t arrive until mid-May.
On April 12, the government fast-tracked emergency approval for foreign vaccines provided they’d been approved in the US, UK, or Japan, or pre-qualified by the WHO. Finally, on April 19, the government agreed to grant the Serum Institute about US$400 million and about half that to Bharat Biotech, this in response to a six- month-old appeal, from both companies, for funding to build more capacity.
The government changed its pricing strategy, too, allowing manufacturers to take half their product and negotiate prices with state governments and private hospitals, while keeping the central government’s prices fixed. The Serum Institute announced it would charge 400 rupees per dose to state governments and 600 rupees to private hospitals. Opposition parties promptly accused the company of profiteering and the central government of following a discriminatory policy—even though vaccines had previously been sold below cost, harming the manufacturer. Everyone conveniently forgot this point or never understood in the first place. As it has over and over during this crisis, the government found itself in a no-win situation. By this point, though, the damage was done. India had withstood the first wave of the coronavirus admirably, but now its fate was sealed.
To make things worse, US trade regulations make it all but impossible to export critical components for manufacturing vaccines. On April 20, the CEO of the Serum Institute, Adar Poonawalla, took to Twitter to beg President Biden to lift the export embargo on raw materials. US officials claim there is no embargo, as such. But this is the impact of laws like the Defense Production Act, which oblige US manufacturers to prioritize federal orders. Manufacturers outside of the US correspondingly suffer.
Vaccinate the world
If the US was operating with a more rational concept of its defense requirements, it would remember how pandemics work. If India’s second wave is not brought under control, quickly, its mutants will spread to the world, the US included. It is a simple biological fact that the pandemic is not over for anyone until it’s over for everyone. For India, it is emphatically not over.
As the Cosmopolitan Globalists have argued—at length—the United States is the only country that could end the pandemic. As India’s tragedy demonstrates, it must. No one else can. No one else will. There is no time to waste.
The vaccines in use in India are the two-dose Covaxin vaccine, based on the old-fashioned, tried-but-true technology (dead coronaviruses), and Covishield, which is the two-dose Oxford-AstraZeneca vaccine, prudently renamed.




I have actually disagreed with the Cosmopolitan Globalists for a long time that the US is the ONLY country that can end the pandemic. I do think trying to end the pandemic without the US i.e. just relying on vaccine supply chains predominately in the EU and some other countries is profoundly risky, dangerous, and stupid, however, it appears the Biden Administration actually wants to try to "test" this possible option. I guess the question I have for other Americans is what exactly is the benefit for America in doing this. If the rest of the world is somehow able to take care of this on their own a certain degree of what Madeline Albright used to call "the indispensable" nation will be gone never to return.
In conclusion, I do feel as if the clock is ticking. If Biden at the 11th hour releases the vaccines for export I sure many including even CG's like Claire and Vivek might praise "America to the rescue" but by then I am not sure the facts on the will warrant such a conclusion in fact we might have already passed this point.
**I guess a corollary is if up to this point the world had only relied on the United States without the EU we would actually all probably be dead by this point so perhaps one might say the European Union is the only entity at least keeping most of us still alive.
Honestly, your description of the political environment in India makes the US sound like we're at an Oxford debate. This is terrifying. How the hell are rational voices supposed to penetrate that maelstrom of disinformation and political framing of every issue? We can't do that (see below) and we're not nearly as bad off.